the scalloped appearance of the gums where they meet the teeth. b. a design carved on the base material of a denture to simulate this.
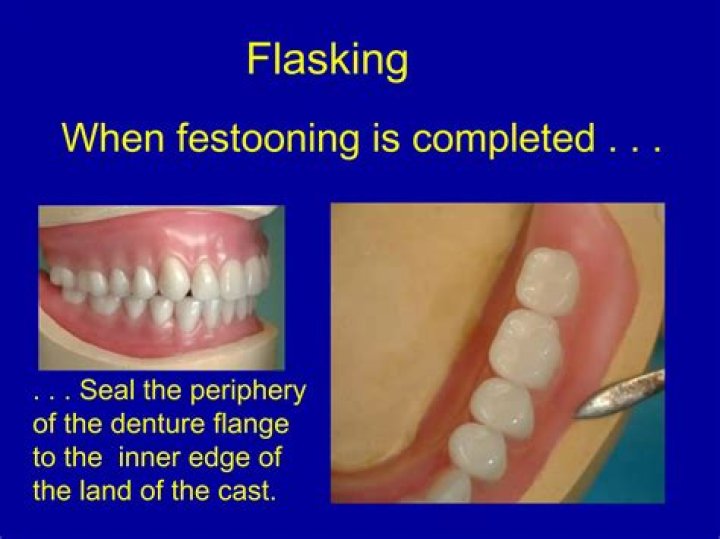
What is festooning a denture?
Figure 5 The wax is flowed into position with a warm spatula after the wax has been dripped onto the denture base. The objective of either the “drip-on” or “press-on” method is to add a sufficient bulk of wax to the denture base which can then be carved to the proper contours. …
What is edematous gingiva?
Enlargement of marginal and interproximal gingival tissues. Results from collagen loss and an accumulation of interstitial fluid. Tissues are easily compressed with a blunt instrument. Diffuse redness.
What does gingival margin mean?
The free gingival margin is the area located between the sulcular epithelium and the epithelium of the oral cavity. This interface exists at the most coronal point of the gingiva, which is also known as the crest of the marginal gingiva. The gingival margin (F) is the most coronal point of the gingiva.What does fibrotic gingiva mean?
The term is fibrotic. Fibrotic gingiva is described as “hyperkeratinized [tissue] with an abnormal whitish thickening of the keratin layer of the epithelium.”1 The problem is that, at first glance, it appears light in color and “firm” to the touch.
What causes stippling in gingiva?
Stippling occurs as a result of the microscopic elevations and depressions of the surface of the gingival tissue due to the connective tissue projections within the tissue. The degree of keratinization and the prominence of stippling appear to be connected.
How many types of gingiva are there?
Structure of the Gingiva There are two types of gingiva and several important anatomic regions. Alveolar mucosa – The area of tissue beyond the mucogingival junction. It seems less firmly attached and redder than the attached gingiva.
Is gingival margin the same as recession?
Gingival recession, also known as receding gums, is the exposure in the roots of the teeth caused by a loss of gum tissue and/or retraction of the gingival margin from the crown of the teeth.Where is gingival margin?
The free gingival margin is the area located in between the sulcular epithelium and the epithelium of the oral cavity. This interface exists at the most coronal point of the gingiva. This is also referred to as the crest of the marginal gingiva.
What is gingival margin measurement?Gingival Margin is the area of the gingiva closest to the tooth surface, commonly referred to as the ‘gum line’. -GM reflects recession of the gum line. -GM measures from the Cemento-Enamel Junction (CEJ). … -GM is assigned a negative value of 1-10 when the gumline is above the CEJ.
Article first time published onWhat is gingiva?
(JIN-jih-vuh) The tissue of the upper and lower jaws that surrounds the base of the teeth. Also called gums.
What causes bulbous gingiva?
Gingival enlargement can be induced by three main causes stemming from (1) inflammation, (2) medication, and (3) systemic disease. Treatment can be in the form of allowing for spontaneous resolution once the etiology is removed, instituting proper dental hygiene, nonsurgical treatment, and/or surgical treatment.
What is gingival polyp?
Objective: Gingival Polyp, which are focal fibrous hyperplastic lesion, are also known as, localized gingival enlargement. Represent a reactive hyperplasia of fibrous connective tissue in response of trauma or irritation.
What causes gingival fibromatosis?
Gingival fibromatosis can be caused by number of factors including inflammation, leukemic infiltration, and use of medications such as phenytoin, cyclosporine or nifedipine,[14] and vigabatrin. [19] Gingival enlargement can be part of Laband, Rutherford, Ramon, or Cross syndrome.
What bacteria causes acute necrotizing ulcerative gingivitis?
If ANUG is improperly treated or neglected, it may become chronic and/or recurrent. The causative organisms are mostly anaerobic bacteria, particularly Fusobacteria and spirochete species.
What is Fibrosis made of?
Fibrosis is defined by the excessive accumulation of fibrous connective tissue (components of the extracellular matrix (ECM) such as collagen and fibronectin) in and around inflamed or damaged tissue, which can lead to permanent scarring, organ malfunction and, ultimately, death, as seen in end-stage liver disease, …
What is the function of gingiva?
The gingiva (or gums) is the tissue that surrounds and protects the teeth and underlying bone. The gingiva is attached to the tooth, forming a seal that protects the underlying bone and helps provide a barrier against infection.
Is gingiva part of oral mucosa?
Clinical Presentation and Pertinent Anatomy. The gingiva is part of the masticatory mucosa that provides an internal defense mechanism against pathogens and mechanical stress. It is composed of a dense, vascular fibrous tissue with a keratinized stratified squamous epithelium.
Why gingiva is coral pink in color?
What color is the human gingiva? It is frequently described as “coral pink” and is dependent upon the thickness of epithelium, the degree of keratinization, the magnitude of pigmentation, and the underlying vascularization1.
Is stippling in gingiva healthy?
Stippling was thought to indicate good gingival health, but it has since been shown that smooth gingiva is not an indication of disease, unless it is smooth due to loss of previously existing stippling.
Why is stippling absent gingivitis?
Because the attached gingiva is dense, firm, and tightly attached via the collagen fibers of the connective tissue to the cementum and alveolar bone, stippling is typically seen. Not everyone will show the presence of stippling and those that do, may show varying degrees of stippling within their own mouth.
Why normal gingiva is not identical with clinically healthy gingiva?
The gingival sulcus, or crevice, is therefore created between tooth and mucosa; its depth varies from 0.1 to 0.3 cm. The attached gingiva extends from the free gingival groove to the beginning of the alveolar crest and is continuous with the alveolar mucosa.
Why is attached gingiva important?
Historically, the presence of a wide zone of attached gingiva has been considered beneficial, as the gingiva plays an important role in maintaining the periodontium in health. It provides a physical barrier to oral biofilm, dissipates masticatory forces and protects the periodontium from injury.
What is sub gingival calculus?
Subgingival calculus refers to calculus below the crest of the marginal gingiva which is not readily visible upon oral examination. It is usually dense and hard, dark- brown or green-black in color, flint-like in consistency, flattened in shape, and firmly attached to the tooth sur face ( s ) .
What is a gingival margin trimmer?
Margin trimmers, also known as gingival margin trimmers, are restorative cutting instruments used to cut enamel and produce a bevel on enamel margins. These dental instruments have slightly curved blades with sharp beveled cutting edges to provide mesial or distal access into the preparation.
What is the treatment for gingival recession?
Many techniques have been introduced to treat gingival recession, including connective tissue grafting, or CTG; various flap designs; orthodontics; and guided tissue regeneration, or GTR. The authors reviewed human clinical studies to assess which techniques provided optimal results.
Is gingival recession reversible?
Unfortunately, gum recession cannot be reversed. The tissue will not grow back but there are specific steps to take to keep the recession from getting worse. Successful treatment ultimately depends on how your gum recession originated in the first place.
Is gingival recession painful?
Receding gums, or gum recession, essentially means that your gum tissue has started to pull away from your teeth, exposing the roots. Once tooth roots are exposed, they’re left unprotected from the elements including hot and cold beverages – and maybe even your toothbrush. The result is shooting sensitive tooth pain.
How is gingival overgrowth measured?
- When recession of the gingival margin is present, the CAL is calculated by adding the probing depth to the gingival margin level. …
- When the gingival margin is coronal to the CEJ, the CAL is calculated by subtracting the gingival margin level from the probing depth.
How do you measure gingival recession?
Gingival recession is measured clinically as the distance from the cemento-enamel junction to the depth of the free gingival margin using the millimeter markings on the periodontal probe and reflects exposure of the root cementum [7, 8].
What is a gingival index?
The Gingival Index (GI) scores each site on a 0 to 3 scale, with 0 being normal and 3 being severe inflammation characterized by edema, redness, swelling, and spontaneous bleeding4 (Table 2-2). This measurement is based on the presence or absence of bleeding on gentle probing.